Arthritis is an inflammatory condition of joints. There are several types of arthritis. The most common type is osteoarthritis or wear-and-tear arthritis that affects the joint at the base of the thumb. Thumb arthritis is more common in women than men, and usually occurs after the age of 40 years. Patients who have arthritis of the fingers may have swelling, pain, stiffness, and deformity all of which interfere with the use of the hand. Base of thumb arthritis is also called 1st CMC joint arthritis (1st carpometacarpal joint arthritis) or TMC arthritis (trapeziometacarpal arthritis)
Diagnosis of thumb arthritis is made by examining the thumb. X-rays of the joint may be taken to know the severity of the disease and to determine whether there are any bone spurs or calcium deposits.

Nonsurgical treatment methods for relieving pain in an arthritic joint include activity modification, pain medications, and use of splints, and steroid injections.


Surgery is usually considered if nonsurgical treatment fails to give relief. There are different surgical procedures that can be used and may include:
Synovectomy: This surgery is usually indicated for early cases of inflammatory arthritis where there is significant swelling (synovitis) that is causing pain or is limiting the range of motion of digits and thumb. Synovectomy is a surgical removal of the inflamed synovium (tissue lining the joint).
Trapeziectomy and Thumb suspensionplasty/ Ligament Reconstruction and Tendon Interposition (LRTI): In this procedure, Dr Bala approaches the base of the thumb from the back unlike many other surgeons. This approach involves careful dissection of tendons and nerves and meticulously raising tissue flaps that can be sown back later. The thumb contracture is first released. An important blood vessel is carefully dissected out to avoid injury. Dr Bala uses special magnification loupes to visualize and protect individual blood vessels and nerves in this region to minimize complications.
He removes the affected joint (trapeziectomy) taking care to preserve the tendon deep to this joint. He replaces the removed portion of the joint with a portion of the tendon harvested from the front of the wrist and passed through to the back of the thumb. This tendon is passed through the base of the thumb bone to stabilise the joint (dynamic suspensionplasty), wound around its own stump and interposed between the joint surfaces. This is a dynamic stabilisation procedure devised by his mentor Prof Mah from Flinders University Adelaide, South Australia. Sometimes the small joints near the base of the thumb (ST joint arthritis) which are also arthritic along with the basal joint of the thumb can be a cause of persistent pain even after this surgery, if not addressed. Dr Bala prefers to fuse these joints (ST joint fusion) with the bone removed from the base of the thumb if found arthritic during surgery. He prefers to use an implant called a staple to fuse this joint.
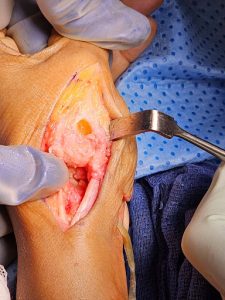
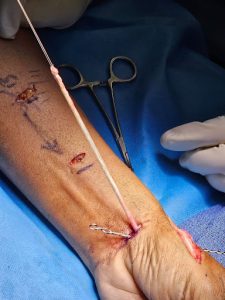
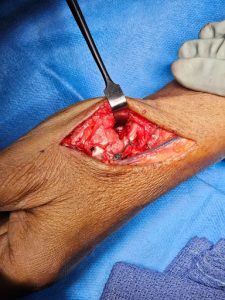

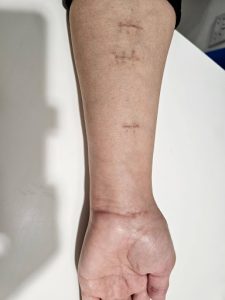
Trapeziectomy and the internal brace procedure: A more recent technique for addressing the base of thumb arthritis is removing the trapezium which is worn out and suspending base of the thumb to 2nd metacarpal (2nd hand bone) by means of a device called the tightrope or similar. Dr Bala is waiting to assess long term results of this procedure before recommending this as one of the options for his patients.

Arthrodesis: A fusion, also called an arthrodesis involves removal of the joint surfaces and fusing the bones of the joint together using metal plates, screws or staples. Even though this surgery eliminates all motion at the base of the thumb, the resulting fusion is very strong and in a functional position.
This surgery is usually indicated when the joints are severely damaged, when there is limited mobility, damage to the surrounding ligaments and tendons, failed previous arthroplasty ( base of thumb replacement/ 1st CMC replacement or TMC replacement), or when heavy manual use is expected.

Arthroplasty: This is a more recent addition to the armamentarium of options that are available for treatment of this condition. Dr Bala would like to wait for long term results of this procedure before recommending it for his patients. Dr Bala has attended cadaver workshops to perform this procedure.


Dr Bala will discuss with you the options and help you decide which type of surgery is the most appropriate for you.
Rehabilitation
Following surgery, a rehabilitation program, often involving a physiotherapist may help to regain hand strength and movement. You may need to use a post-operative splint for a while after surgery that helps to protect the hand while it heals. You may need to restrict activities for 12 weeks to let the joint reconstruction heal properly. Although recovery is slow, you should be able to resume your normal activities within a few months of surgery.
